
With restrictions eased, public health warnings muted and mask wearing now almost non-existent, the risk of contracting covid-19 is still very real, particularly as people come together for Christmas parties and family gatherings.
Daily covid-19 numbers are the highest they have been for four-and-a-half months.
Immunologist Dr Anna Brooks of the University of Auckland says she is gravely concerned at the cavalier approach hundreds of thousands of New Zealanders are now taking to covid, particularly thinking that if they have already had it, they are not at risk of reinfection.
Dr Brooks tells Kathryn Ryan about how New Zealand is coping with the pandemic’s enduring impact and looks ahead to what could be a deadly summer of reinfection.
Kathryn Ryan: What is going on at the moment with this rise in reported cases? Are we in another surge of covid?
Dr Anna Brooks: Yes, that absolutely seems to be the case.
These variants that are circulating have a better chance of infecting us because they’re evading our immune defences and so reinfections are going to be far more common than we’ve experienced for example, in the second wave.
So, there might be a bit more complacency because we’ve had two waves and people may have thought, “Well, I had it once I didn’t get it again,” and that’s really just not the case.
These variants, there’s a whole bunch of them out there and many of them we actually won’t even know exist because of the low level of data collection and variant tracking.
New subvariants
KR: We’re getting new subvariants; just explain what that means for your existing level of protection, either from previous infection and/or from vaccination — these subvariants will be better at evading than what we had before.
AB: Exactly. What’s happening is as each new variant or subvariant is evolving, it’s doing so to evade our immune protection.
So absolutely, that can be from the vaccinations and/or previous infection.
What we’ve sort of had in our country, is we had that really large first wave, which was the BA.1 and [BA.2]… then the next wave we had was BA.4 and [BA.5], so we’ve got some what we call hybrid immunity within the community, absolutely. But it’s not enough to stop reinfection when the subvariants are still able to skip round our antibody response and infect us.
And as we know, our vaccinations are a great starting point for preventing severe illness but they’re not great at preventing infection. So, if these variants are capable of infecting any of us, regardless of our baseline immunity, then we’re going to see cases rise, we’re going to see severe illness and hospitalisations and deaths again — that’s the facts.
Impact of reinfection
KR: Can we talk about reinfection? Because I think people have had that sense of, ‘I’ve had it, so I’ve got a few months free now.’ But is there also a sense of, ‘I’ve had it and I didn’t have any major issues, so I’ll be fine next time too.’ Can you explain what we’re learning about the impact of reinfection and what to assume, or rather not to assume?
AB: I think that’s exactly right. I think there’s a general feel that if you’ve had covid, you survived it perfectly fine, that if you get it again, it’ll be the same.
But what we’re seeing coming through the literature — and these are really large-scale studies that have been tracking reinfections — is that each infection or reinfection is increasing your health harms or your risk of health harms.
So, that’s where we really want to raise awareness right now, that people aren’t complacent about the fact that just because they’ve had at once, they’re not at risk, because everyone is at risk.
What we don’t understand is how long the body takes to get back to what I call a baseline level of [recovery in the body] and you won’t necessarily feel that. You may have had your infection, it may have been very mild and you’re like, ‘Yeah, that was nothing.’ But it’s not really nothing if you then go and get another reinfection, and then another one on top of that.
We don’t really know, especially now there are so many variants circulating, we just don’t know what the risk factors are and even the ability… to get exposure to multiple variants over a short period of time.
The literature is telling us each infection is risky, and reinfections increase that risk. Some of the publications are suggesting that that risk lasts for at least six months and that those are risks of heart attacks, strokes, clotting events, all those things that nobody wants as a risk factor.
Inflammation risk
KR: Just explain again why inflammation, that elevated immune response and why inflammation associated with it is a risk factor for long covid?
AB: What we understand from all the research that’s going on is that, first of all, this virus is not just a respiratory virus.
That was where the first level of complacency crept in, when we started to see less respiratory failure, and the lung issues, and kicked off with Omicron.
But essentially, Omicron has been a different beast, and remains that way. What we do know is that it still has the ability to impact our blood vessels, our blood vessels feed all our organs.
Part of the immune response when we get infected, we know that the virus can cause clotting issues, and that probably happens in all of us. It’s part of an immune response to form clots to get the infection under control and perhaps what’s going on is that some of us resolve that inflammation and that clotting, and we all go back to normal, and in others, that doesn’t happen.
And that’s just one part of the picture. What I believe a lot of the literature is pointing towards — and it is one of the hypotheses we’re chasing down — is also that your immune system has had a hammering to a certain extent and we don’t know how to actually detect that, we don’t know how long it takes to resolve, but it kind of puts us all in a slightly vulnerable position.
What we are starting to see more coming through, and again, as I say, as part of the research we’re looking into, is that it disrupts our immune control of what we are wandering around with every day and that’s all our microbiome, and including latent or dormant viruses that we got in childhood, that live with us for life.
Some of the research is indicating that we get a reawakening of our viruses and some of the ones that are well known are chickenpox. Many of us get chickenpox, and then we get shingles. When our immune system — our immune control — breaks down, we get an outbreak of shingles because the shingles presentation, if you like, indicated that you had chickenpox as a child.
Epstein-Barr virus
That’s one virus we know, the other one that is kind of front and centre that everyone’s chasing down a bit more is Epstein-Barr virus. So this is EBV, or what we know of as glandular fever, and most of us are exposed to this.
The numbers are around at least 90 percent of us wander around controlling EBV dormantly… but at the same time, we know that not everyone gets severely impacted by EBV.
We’re starting to wonder whether it’s viruses like that, that inhibit us all, that are getting reawakened through a loss of immune control. And that could be contributing to what we now know as post-viral illnesses because, obviously, long covid is front and centre because this pandemic is uncovering that, but it also loops into myalgic encephalomyelitis or chronic fatigue syndrome.
EBV has been a strong contender as being a cause of that illness too, so it’s really showing us that we haven’t done enough research into understanding how our immune systems wonderfully control latent viruses or dormant viruses that we contract as youth, as children, and maybe that’s part of the picture here.
KR: So the question now is, what is it you can do to go forth and have a fabulous Christmas, a good holiday, enjoy life as fully as possible but still manage this continuing risk?
AB: We all want to have fun in summer and gatherings and all the rest of it. My main message at the moment is that I want to make sure people understand that there is a risk… and we want people to manage their own risk, but not just their own risk, because vulnerable people are getting more and more shut away, because they no longer feel safe to be anywhere because they’re vulnerable to infection.
Those two things coming together, we’re basically in a position where we’re now essentially being told to look out for our own selves, because there’s very little public health messaging about the risks.
It’s two things here. It’s education that the risk isn’t going away, you want to protect yourself and understand those risks, and know that… any infection comes with a risk and there are people out there that are getting more and more concerned about their health not being taken seriously, because people around them don’t care anymore…
Keeping businesses open
I think some simple measures will keep businesses open too… You know, quite often when we’re raising awareness you feel like it’s the economy or businesses that are like, ‘Oh, make covid go away.’ We’re actually raising this awareness to keep businesses open. We want businesses to thrive over summer, but if there are no health protections in place, and you have customers in enclosed spaces, and your staff are getting infected, you’ll have no staff, you can’t open and so on and so forth.
I think the most obvious one is flying and public transport… if we’re not masking on planes, is that a ticking time bomb before there are no staff and you can’t get to your holiday destination?
KR: Back to your other key point, which is that reinfection being the trend possibly of the summer, those rates are getting quite high… are they getting close to a third of new cases being reinfections?
AB: Yeah, it looks that way. We have to remember that without a surveillance programme of you know, random testing, we have actually very little intel on what that number is going to be.
[If] we’re not collecting random data, then we have no idea how much asymptomatic spreads happening or how many people are getting infections.
We can’t forget about that. We need to remember that that is why we RAT before an event, that is why we RAT before we go to a Christmas function. It’s not just because you’ve got symptoms — we don’t know how many people are getting asymptomatic infections.
That’s now become an individual choice, whether you do that, because it’s not part of any public health messaging that you should check to make sure you’re not asymptomatic.
So, if we don’t know how many people are out there asymptomatic, they’re not going to be testing, they’re not going to be reporting, and then they won’t even know if in a month, two months’ time they get an infection, whether that’s a reinfection.
That’s what we would love to see from a scientific position, and, you know, safety and understanding all of our risks, is actually gathering data so we can understand this and that includes knowing what variants are out there.
Every time around immune system is waning, depending on how long ago we were infected, or boosted or vaccinated, then the chances of our illness…being worse is going to increase as well. So severity, risks increase the further ago your immune response was.
RAT tests and variants
KR: Are the RAT tests just as effective with the new variants?
AB: We’ve heard that the RATs are picking up the variants. It’s only as good as how good the person is testing as well.
KR: Are the boosters keeping up with the variants?
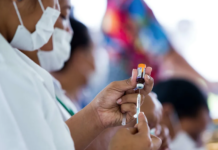
AR: Boosting revives your immune system… the data showed any boost is going to give you that little bit more protection, because what it’s doing is training the immune system, and it’s reviving it, it’s waking it up, and you’ve got more circulating antibodies. They might not be perfect at shutting down the variant that you get infected with, but it’s going to do a better job than being completely non-boosted.
But what we’d like see is, there are the bivalent vaccination boosters that will protect you more against the BA.4 and [BA.5] strains. And essentially what we really need is a new generation of vaccines that sterilises and stops infections.
This article is republished under a community partnership agreement with RNZ.



![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-218x150.png)






























![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-100x70.png)






