
New Zealand’s Director-General of Health Dr Ashley Bloomfield says it is clear that the number of cases in Auckland is on the way down, but in Wellington case rates are increasing rapidly.
Dr Bloomfield and Chief Science Advisor Dr Ian Town held a media briefing on the Omicron response today.
Dr Bloomfield said there were 21,616 new cases of covid-19 in the community and 960 people were in hospital, including 22 cases in ICU or high-dependency units with two more deaths.
- READ MORE: Covid-19 update: Two more deaths, 21,616 new community cases and 960 people in hospital
- Declining NZ covid-19 case counts – but record deaths and more to come
- Other NZ covid outbreak reports
In the Northern region there were 559 people in hospital, with 40 percent — some 233 — aged 70 or over, he said.
Dr Bloomfield said the country saw higher case numbers compared to modelling from before the outbreak, but it was clear that the number of cases in Auckland is on the way down.
There were 6085 new cases in Auckland today, up from 4730 yesterday and 4509 on Sunday.
Dr Bloomfield says while admissions were on the way down, the total number of people in hospital with covid-19 was continuing to increase. Peak hospitalisations typically lagged behind peak case numbers by about a week.
Shift to subvariant BA.2
He said New Zealand had seen an interesting shift to the omicron BA.2 subvariant rather than the BA.1 variant. This could help explain why there were more transmissions than expected in the high-transmission scenario modelling.
However, this may be in New Zealand’s favour because other jurisdictions overseas — for example, NSW and the UK, particularly Scotland — were seeing second outbreaks with the BA.2 variant, having already had BA.1 variant outbreaks.
He said Scotland was seeing its highest case rate in nearly two years and had about 1800 people in hospital with the variant, compared to the under 1000 in New Zealand. Scotland has a population of 5.4 million, comparable to New Zealand’s 5 million.
Watch the update:
Video: RNZ News
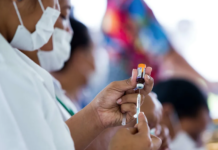
Dr Bloomfield said it was important to make sure people were “vaxxed to the max”. He said this was a change in language — where the previously talked about term “fully vaccinated” was two doses, it was a shift to talking about being up to date with vaccinations.
He said it was clear that protection against getting omicron and/or being hospitalised wanes over time with just two doses.
A report from the Northern Region from March 8 showed just 16 percent of people admitted to hospital had their booster more than two weeks prior.
“So fully 84 percent of those people were not fully boosted … so even though only a small proportion of our population now has not had two vaccinations it is really really clear that a booster protects people from being hospitalised and we know it also helps protect people from dying from omicron.”
He said that in the same two weeks prior to March 8, just one person admitted to ICU was fully boosted.
Wellington outbreak
Dr Bloomfield noted there was now a “pretty full on outbreak” in Wellington, with case rates increasing rapidly.
But he thought the outbreak in Wellington, including the Hutt Valley and Kāpiti Coast, had yet to peak.
There were 1584 cases in the Capital and Coast DHB catchment and 33 hospitalisations.
“I think the rate of increase is similar to what we may have seen in Auckland, Waikato, Bay of Plenty and others beforehand.’
Dr Bloomfield said the region with the highest case rate — per capita — right now was Tairāwhiti.
He said the DHBs (district health boards) had good plans in place, but when they had particularly high case numbers in hospital they did need to scale back some of their normal services.
He said some people were returning several negative RATs, but RATS were just “one tool” and not as accurate as PCR tests. He said people who had symptoms should assume they have covid-19.
Long covid
Dr Ian Town talked about long covid. He said most people who developed covid recovered completely, but the term “long covid” was generally applied to people who continued to suffer effects for at least 12 weeks.
It can include low energy, fatigue, shortness of breath and cough, headaches, low mood, difficulty concentrating, cognitive impairment, ongoing chest pains, a racing pulse, joint pains, aches and pains, weakness in muscle, ongoing changes to sense of taste or smell, and poor quality of sleep.
Dr Town said there was no suggestion the symptoms of long covid were psychological symptoms, and the key thing was to pace yourself and accept that more rest may be needed.
There was no specific treatment, but it was thought to be part of a post-viral immune response and the approach to long covid was “very much a framework of rehabilitation and pacing yourself and not overdoing it”.
“There isn’t a magic bullet in terms of the recovery.”
This article is republished under a community partnership agreement with RNZ.


![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-218x150.png)






























![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-100x70.png)







