
By Jamie Tahana, RNZ Pacific journalist
When Max Manape received the confirmation in Papua New Guinea his heart sank. A 22-month-old girl had been diagnosed with polio. She was paralysed.
A few days later, another confirmation came. A two-year-old boy had been taken to a clinic with weakness in his legs. Workers sent away for testing and he, too, was found to have polio. He’s undergoing physio treatment, but the virus is incurable.
“When the polio was identified, oh it was quite worrying,” Dr Manape sighed down the phone. “We thought we had eradicated it.”
READ MORE: A ‘lurking beast’: Polio casts shadow over PNG independence day
Dr Manape, who is the head of the Eastern Highlands Provincial Health Authority, has since received confirmation that four children in his province have polio.
In all, 12 children across Papua New Guinea have been diagnosed since it was rediscovered in July. The debilitating disease is in five provinces, including the capital, Port Moresby.
Polio, an incurable virus which causes paralysis in children, has been nearly eradicated from the face of the earth. Only three countries – Pakistan, Afghanistan and Nigeria – are still known to harbour wild polio virus, according to the Global Polio Eradication Initiative.
In 2017, only 22 cases of polio came to the attention of authorities worldwide. Papua New Guinea’s latest outbreak has already confirmed 12, and officials there say several more are likely to be found.
3 other countries
Syria, Somalia and Democratic Republic of Congo are the only other countries to have seen a return of polio in the past couple of years.
The government and health officials, in a series of statements and television appearances, have sought to allay fears, saying the outbreak can still be contained by the intensive isolation and vaccination campaign that is underway.
But as confirmed polio cases skip from province to province, many are asking how Papua New Guinea has become one of the few countries to buck the international trend of eradicating polio.
“Everyone’s asking that question,” said Luo Dapeng, the World Health Organisation’s representative in PNG. “I think there’s a multitude of reasons.”
Papua New Guinea, along with the rest of the Western Pacific, was declared free of polio in 2000. Its last confirmed case was in 1996, after decades of intensive vaccinations across the country – and the world.
“I think we got a bit more relaxed in terms of our vaccine programme,” said Dr Manape.
But that confidence was shattered in May when a 6-year-old boy from Lufa Mountain, a settlement in the northern city of Lae, became paralysed in his lower limbs.
Vaccine-derived form
Samples were sent to the United States for testing, and in June, fears were confirmed: Polio was back.
The Lae case is what is known as a vaccine-derived form of polio, where the weakened form of the virus used in vaccinations mutates and spreads. Samples of other children in Lufa Mountain confirmed they had the strain in their systems.
Often, one confirmed case of paralysis is considered a polio outbreak, as doctors assume hundreds of others would have been exposed to the virus.
Lufa Mountain, like much of Papua New Guinea, had the perfect conditions for an outbreak. Few children are immunised against polio, and the water supply and sanitation systems are largely non-existent.
Authorities suspect the outbreak started when the water supply was contaminated by faeces which contained the mutated virus.
Since then, the disease has skipped from Morobe province to neighbouring Madang. It’s spread up the rugged Highland interior to Enga and Eastern Highlands provinces. Last week, the first case was confirmed in the capital, Port Moresby.

Dr Manape said it was not yet known how the virus managed to skip up to Eastern Highlands from Lufa Mountain. He doesn’t even know if it’s from the same outbreak.
“It’s quite worrying,” he said. “We have low vaccine coverage in the province. When we detect polio, it’s quite worrying.”
Geographic spread
Dr Manape said there was a chance polio had been circulating in his province for some time. The four cases found in Eastern Highlands are geographically spread across the province, and a strain could have been there for “quite a while.” It was only once the case was confirmed in Lufa Mountain that they started testing in his region, he said.
“With poor sanitation and the poor water, we know that this could affect every community,” Dr Manape said. “We’re on our toes trying to get to communities, to mobilise health staff.”
David Mills, a doctor in Enga Province and the president of the Society of Rural and Remote Health, said now an outbreak had started, it would be difficult to contain.
“If you leave the door even just a little bit open it can kick it wide open,” he said. “Once you get one case, then one case is all it takes for it to spread like wildfire and then you’re sort of back to step one again.”
Since the outbreak was confirmed, an army of health professionals have swarmed the country, marching from village to village to vaccinate as many children as possible and contain the outbreak.

The World Health Organisation and the Department of Health have set up containment zones around affected communities, and embarked on mass vaccination campaigns across the provinces with polio.
In some of the provinces, Dr Dapeng said, coverage has already gone from as low as 30 percent to as high as 90 percent.
More than 50 deployed
More than 50 international polio workers have been deployed to the country, according to the World Health Organisation. A vaccination campaign will begin in Port Moresby at the end of the month, while a nationwide campaign will begin in October. Last week, health secretary Pascoe Kase said the immunisation programme would also be expanded to include all Papua New Guineans under the age of 15.
But while the response is being lauded, many are saying it could have been avoided entirely.
“To see this re-emerge is very disappointing,” said Dr Mills. “But perhaps not altogether surprising.”
“When you see these diseases re-emerge, it really is a sign that unfortunately the government has not really invested in these things.”
Polio’s return was years in the making.
In the late 20th century, vaccination programmes were well-funded and regular. Most villages would be visited by specialists who would traverse the country providing children with their three courses of droplets.
But since the eradication declaration in 2000, Dr Manape and Dr Mills both said, that programme has largely fallen by the wayside, replaced by a lackadaisical approach to vaccines. Not just for polio, but for other preventable diseases like measles and whooping cough, too.
Vaccine coverage down
In the past 18 years, nationwide polio vaccine coverage has fallen from about 80 percent to 30 percent. In some provinces, that rate is even lower.
While some children are vaccinated, they don’t receive their full doses, which also creates a danger. To be fully immunised, a child needs three courses of droplets. But Dr Manape said some children had only been receiving one course, which can spread the mutated virus while not fully vaccinating the child.
“The immunity of the population is very low,” said Dr Luo, of the World Health Organisation. “That’s why polio has come back.”
But the campaign is also the victim of the grand promises, failed visions, and savage cuts that have seen the country’s health system hurtle close to the edge of collapse.
In recent months, hospitals and clinics across the country have run out of basic medicines and supplies, the country almost ran out of the antiretrovirals used to treat those living with HIV/AIDS, and doctors have gone without pay for months.
Dr Luo acknowledged that the financial crisis, in part caused by a spending spree that started when the government was confident of a commodities boom that never came, may have had some role in the return of polio.
“PNG’s a commodity income country and they have been struggling to finance some of the health services,” he said.
Easy target for cuts
Dr Manape said it appeared vaccine programmes – especially ones for ailments like polio, thought to have been eradicated – were easy targets for savage cuts.
“Once we eliminated polio in 2000 we needed to maintain the immunisation coverage – that needs to be constant,” he said. “We do a lot of our planning and send the budgets. The government not funding its part of it has really pulled the cap for the polio to pop up.”
In June, health minister Sir Puka Temu told parliament 40 percent of the country’s remote aid posts, small clinics that treat isolated communities and provide vaccinations, had closed. He said many of those that remained had no electricity or running water.
Dr Mills said in some provinces – including those with polio – nearly all the aid posts had closed, which was “outrageous” in a country where 85 percent of the population lived in remote areas.
He said the government’s spending priorities had been in the wrong places for years, with millions of dollars – much of it donated or on loan from countries like Australia and China – had been pumped into hospitals in the big cities.
“What really needs to change is we need to reinvest in getting health workers living in these communities all the time and that’s really what collapsed in PNG,” said Dr Mills.
“You have to have those people there … so that any time they see a patient, or they see someone at the market they can say, ‘hey look come in for your vaccination tomorrow’.”
Lives changed forever
But after 18 years of cuts and neglect, polio is back, and the lives of 12 children have been forever changed.
Authorities are scrambling to contain the outbreak in a response that has been spearheaded by international agencies which has seen millions of dollars flood in.
Dr Mills said eradicating it again is possible, but the teams working across the country – including himself – have their work cut out for them.
“There’s no power supplies in most of the country and, of course, [that] challenge of keeping in place what we call a cold chain to make sure the vaccines stay cold the whole way to the patient, that’s an incredibly difficult task,” he said.
“You may have to travel a long distance just to vaccinate a couple of dozen children. That might involve flying out or walking a day or taking a motorboat ride up the river for a couple of days just to find small groups.”
“It takes will and effort to do it,” Dr Mills said.
Dr Luo said that will and effort was there, and he was confident the polio outbreak could be contained.
Know the strategy
“We know the strategy of how to do it. We know how to do surveillance. We know how to implement the intervention,” he said. “We will someday contain the outbreak.”
Medical workers are already looking beyond the containment effort, and are demanding assurances that the problems that led to polio returning will be fixed, and that vaccinations will be maintained.
“With the WHO resources and funding we’re having coverage of almost 100 percent,” said Dr Manape. “But for our normal routine, that funding was a big problem. What we are learning now is that we need more support from the government.”
Dr Mills said plenty of other countries with similar challenges to PNG had managed to stay on top of polio, and he hoped lessons would be learned.
“Let’s hope this provides the impetus to refocus our attention on these basic things.”
This article is republished under the Pacific Media Centre’s content partnership with Radio New Zealand.









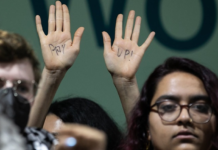



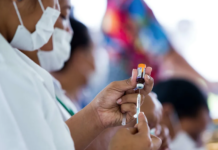




























[…] to New Zealand’s Asia Pacific Report, nationwide polio vaccine coverage dropped in recent years. Since eradication was declared, […]
Comments are closed.