
By Rowan Quinn, RNZ News health correspondent
One year on from Aotearoa New Zealand’s longest covid-19 lockdown, an epidemiologist says further lockdowns cannot be ruled out, instead preparing to do them better.
On 17 August 2021, New Zealand went to alert level 4 because the deadly delta variant had arrived.
Aucklanders had no idea that day that they would still be in lockdown until December, and that after 18 months of trying to keep covid-19 out, it would be here to stay.
- READ MORE: Covid-19 update in NZ: 16 further deaths, 4489 new community cases
- Other NZ covid reports
The city was asked to hold the line so the country could get vaccinated, something critics said should have happened much earlier.
Auckland University epidemiologist Professor Rod Jackson was vocal in urging the country to aim high and vaccinate more than 95 percent of eligible people.
Reflecting back, he said New Zealanders responded well, with most areas hitting that mark or higher by the measurements at the time.
Much had been learnt about the virus — and how to respond to it — since then, with the highly contagious but less harmful omicron variant changing everything at the start of this year, he said.
But the danger was not over.
Random severity of variants
“I think there are a lot of people who think, ‘oh look, it’s getting less severe over time so we’re fine,’ but it’s pretty random whether the next variant is going to be less severe or not,” he said.
Either way, it would need to be at least as spreadable as omicron to take over, he said.

The government has said lockdowns are not part of any future covid-19 plans, with the traffic light system taking its place.
But Professor Jackson said that may not “cut the mustard” if the worst happened.
“If we get a new mutation that is more severe, that kills more people, then we’ve got something huge to worry about,” he said.
“If that happens, if people start dropping dead in the street like the original version of covid, we will have little choice but to lock down.”
That was why the country still needed to be prepared for the worst, he said.
Frontline of delta outbreak
As an Auckland GP and co-leader of Te Rōpū Whakakaupapa Urutā, Dr Rawiri McKree-Jansen was at the frontline of the delta outbreak and lockdown and the vaccine rollout.
Some Māori and Pacific health teams had initially struggled to be given the resources they needed, or to be listened to.
The work they were able to do for their communities and the country showed what they were capable of and should be a lasting legacy, Dr McKree-Jansen said.
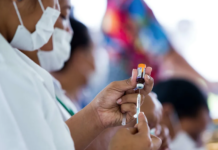
They were crucial to the vaccine roll out and helped the most vulnerable, especially those isolating.
“The mobilisation was impressive, relentless and co-ordinated,” he said.
“Those features are remarkable and give us a great sense of optimism about the contribution that Māori communities and Māori health professionals can make and I hope that is enduring.”
When it came to new variants, he said while it was important to be vigilant about what may come next, it was also important to focus on what was happening now.
“Omicron’s not done with us yet … I’m keen that we don’t forget the lessons we’ve learnt from the Delta and Omicron outbreaks – and supporting communities is fundamental to that.”
Both Professor Jackson and Dr McKree-Jansen acknowledged the people who had died since pandemic began, many more since the omicron outbreak that reached so many people.
But they said they were also grateful that many were protected by the lockdown and the vaccine rollout.
16 more people die
RNZ News reports that another 16 people with covid-19 have died and there are 4489 new community cases today, according to the Ministry of Health.
There are 496 people in hospital, 13 of them are in a high dependency unit
Yesterday the ministry reported another 21 people with covid-19 had died and there were 533 people in hospital, including 12 in intensive care or a high dependency unit.
Deputy Director-General and Public Health Agency head Dr Andrew Old told media this afternoon that modelling from Covid Modelling Aotearoa showed New Zealand was continuing to track at the lower end of what was expected in terms of a second wave this winter.
“We passed a peak in cases earlier that the modelling suggested and now hospitalisations are also declining suggesting these too have peaked. It’s sitting somewhere between 800 and 850 occupied beds across the country in late July,” he said.
Te Whatu Ora-Health New Zealand interim national medical director Dr Pete Watson said the recent drop in covid-19 cases was an encouraging trend.
“By each one of us sticking to public health measures we are making a difference,” he said.
This article is republished under a community partnership agreement with RNZ.






![Israeli claims about an Iran ‘threat’ were always a lie. Now we have proof "That anyone in the White House took this plan seriously, let alone acted on it, is a genuinely staggering notion. But the proposition that [former President Mahmoud Ahmadinejad] could retake the reins of power in Iran is possibly the least preposterous part of the scheme](https://asiapacificreport.nz/wp-content/uploads/2026/06/Mahmoud-Ahmadinejad-WikiP-680wide-218x150.png)






























![Israeli claims about an Iran ‘threat’ were always a lie. Now we have proof "That anyone in the White House took this plan seriously, let alone acted on it, is a genuinely staggering notion. But the proposition that [former President Mahmoud Ahmadinejad] could retake the reins of power in Iran is possibly the least preposterous part of the scheme](https://asiapacificreport.nz/wp-content/uploads/2026/06/Mahmoud-Ahmadinejad-WikiP-680wide-100x70.png)




