By Jake McKee, RNZ News reporter
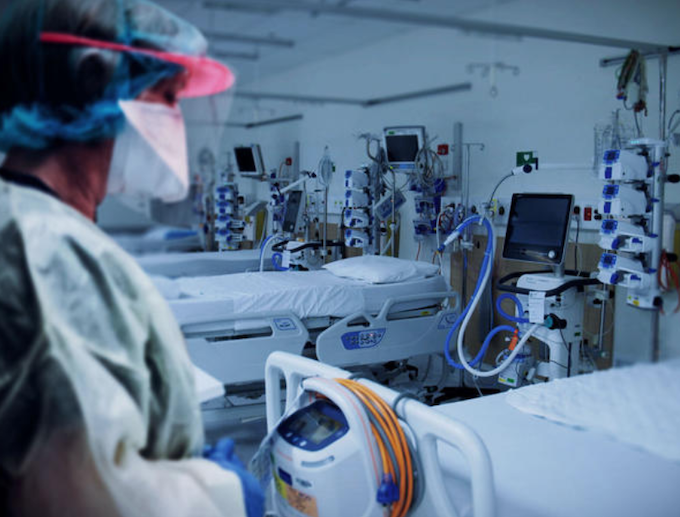
New Zealand’s longest covid-19 hospitalisation in Auckland and Northland during the first three months of the current outbreak was 61 days, and an overwhelming majority of patients were Māori or Pacific.
Figures from the Northern Region Health Coordination Centre (NRHCC) released to RNZ News under the Official Information Act (OIA) show 704 people with covid-19 were admitted to hospital between August 17 and November 18, 2021.
“There were 309 Māori patients, 295 Pacific patients, 36 Asian and the rest [64] were of other ethnicities,” Counties Manukau District Health Board chief executive Margie Apa said in the OIA response.
- READ MORE: Covid-19: Three more omicron cases reported in MIQ
- Boy, 10, is youngest person with covid-19 to die in NZ – MoH data
- 76 new community cases reported in New Zealand
- Other NZ covid outbreak reports
Responding to questions about the response in a statement, a Ministry of Health spokesperson said “protecting Māori and Pacific wellbeing has been an integral part of the ongoing covid-19 response”.
They said the ministry recognised the vulnerability of these communities, “especially given larger family sizes and complex health needs”.
They highlighted how the ministry had redirected $36 million to each of the Māori and Pacific health responses in this current outbreak.
“In addition to providing funding, we remain committed to working with a range of experts, providers, and partners to ensure our response continues to protect Māori and Pacific communities and keeps them safe from covid-19,” the spokesperson said.
‘Unfortunate but predictable’
National Māori Pandemic Group co-leader Dr Sue Crengle said the proportion of Māori and Pacific in the figures was unfortunate but “predictable, given what we know … about how Māori and Pacific communities and whānau are likely to be more vulnerable to transmission of the virus, and also more vulnerable to more severe outcomes”.

She said officials could have learnt and acted faster given the pandemic had been going for more than a year when this outbreak started. But she did note: “we haven’t had a pandemic on this scale since 1918”.
Crengle said there should have been “forward thinking” earlier on.
Apa said there were a total of 870 “patient events” – the difference between this number and the total patient count was because of things like patient transfers between hospitals.
The vast majority — 513 — were unvaccinated, with 124 people having had one jab, and 67 were fully vaccinated.
More than half of admissions (479) were for up to two days, compared with only 73 hospitalisations of 10 days or more.
However, 50 patients ended up in intensive care, seven of them being placed on a ventilator, and on 16 occasions people spent 10 days or more there – including two people who spent 950 hours there, which equated to almost 40 days.
Church deacon
One of those two patients would have been a 50-year-old man, who was a deacon at the Assemblies of God Church of Sāmoa and died in Middlemore Hospital in October.
A caveat of the data in this story was that some people had not been discharged by November 18 – the limit of the OIA request scope.
NHRCC forecasting of “specific hospitalisation predictions” only happened first on October 8, 2021 — more than two-and-a-half months into the outbreak — with the earliest predictions beginning November 9, 2021.
In a graph provided separately by the NHRCC communications team, there were at least three days where intensive care admissions met or were higher-than predicted between November 9 and December 10.
Overall hospitalisations in the same period were always below what NHRCC predicted. NHRCC predicted there would be just under 40 people in hospital in its catchment by 28 December.
Its “specific hospitalisation predictions” did not include modelling on the use of ventilators.
“The use of ventilators is a clinical decision made in response to a patient’s condition and while there are thresholds for use and pathways of care we have not modelled the expected use,” NHRCC said.
More hospitalisations
In contrast to NHRCC, Te Pūnaha Matatini researcher and covid-19 modeller Professor Michael Plank said there had been more hospitalisations than originally expected.
He thought that was likely down to the fact people were being hospitalised “for a shorter stay” so “they have a relatively small impact on the number of beds”.
Dr Plank said intensive care admissions were hard to predict and “to be honest, we haven’t spent a lot of time trying to model that”.
RNZ is awaiting national figures which have been requested from Ministry of Health.
An OIA request to the ministry for national figures was transferred to the NRHCC, a collective of the Northland and Auckland District Health Boards working together on the covid-19 response. National figures have been asked for again.
This article is republished under a community partnership agreement with RNZ.





























![Israeli claims about an Iran ‘threat’ were always a lie. Now we have proof "That anyone in the White House took this plan seriously, let alone acted on it, is a genuinely staggering notion. But the proposition that [former President Mahmoud Ahmadinejad] could retake the reins of power in Iran is possibly the least preposterous part of the scheme](https://asiapacificreport.nz/wp-content/uploads/2026/06/Mahmoud-Ahmadinejad-WikiP-680wide-218x150.png)











