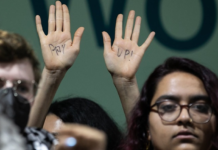Asia Pacific Report newsdesk
The Fiji Women’s Rights Movement warned today that the value of midwives in the Pacific country was being undermined because of a lack of training and proper planning, and little urgency over the creation of positions.
In a message to mark the International Day of the Midwife on May 5, the FWRM highlighted the important role that midwives play in Fiji’s health sector for mothers and their newborn babies.
“The contribution of midwives to universal health coverage in terms of sexual, reproductive, maternal and newborn health, and strategies to fill the service gaps worldwide is rarely mentioned,” said the statement.
- READ MORE: Activist raises concerns about loss of nurses in Fiji
- Fiji nurses resigning because of stress, fatigue and lack of compensation
- Other reports on midwifery
“The barriers they face in their professional environment are not often highlighted.”
More than 65 percent of World Health Organisation (WHO) member states were reported 2020 to have less than 50 nursing and midwifery personnel per 10,000 population (about 40 countries in the WHO African region and 25 in the WHO Americas region).
In many countries, said the statement, nurses and midwives constituted more than 50 percent of the national health workforce.
Pacific data on midwives was limited, the statement said.
Nurses resigning
Earlier this year, Fiji Nursing Association president Dr Alisi Vudiniabola warned that nurses were resigning because of stress, fatigue and lack of compensation.
The same was stressed by Shamima Ali of the Fiji Women’s Crisis Centre.
“We see that nurses are leaving for greener pastures and inexperienced nurses are being promoted to lead units in divisional hospitals which means an impact on service delivery,” said the statement.
In the same article covered by The Fiji Times, Dr Vudiniabola shared a report from one hospital where the nurse manager had been working alone, looking after 28 patients as most of the nurses were “sick and tired”.
“The same is for midwives,” said the FWRM statement. “Midwife training is undertaken with no proper planning or positions being created, or positions are often held up, further undermining the value of midwives and the urgency of their work.”
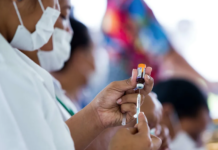
According to the WHO, healthcare provided by midwives who were educated and regulated according to global professional standards was defined as a core strategy for decreasing maternal mortality rates and improving reproductive, maternal, and newborn health.
Midwives could provide 87 percent of sexual, reproductive, and maternal health services but before that can happen, such services needed to be legislated and regulated.
“An enabling environment that allows midwives to offer this full scope of services must be provided.”
Fiji’s commitments
Fiji had made its commitment to Sustainable Development Goals 3 and 4 addressing a reduction in maternal mortality rates but this had not been implemented, said the statement.
Based on reports received, midwives with relevant qualifications like such as the Post Graduate Diploma in Midwifery, Masters in Midwifery were still earning less than F$35,000 a year.
This was the case even when the scope of their work covered areas such as ante-natal clinic consultation, public awareness, births and deliveries, post-natal, retrieval of obstetric and gynecology emergencies in the field (usually handled by doctors), pediatrics, maternal child health, and public health (including immunisation to pre-school for the child).
Midwives also undertake administrative documentation, including maintenance of data repositories, which were not used by the Ministry of Economy in formulating national budgets.
As health communities in Fiji and globally marked International Midwives’ Day today, the FWRM urged the government and the health ministry to place more emphasis on the role of midwives in the health sector.
Queen’s Service Medal for NZ midwife
In New Zealand, midwives’ advocacy was marked on International Midwives’ Day when the Governor-General, Dame Cindy Kiro, presented Pukekohe midwife Claire Eyes with the Queen’s Service Medal at a Government House investiture ceremony which also recognised several covid-19 pandemic response and other service leaders.
Eyes had also assisted midwifery in the Pacific through Rotary and had organised leadership training for midwives and nurses in Australia.
Her citation said in part: “[Claire Eyes] helped prevent closure of the Pukekohe Maternity Unit in the 1990s and secured funding to start the Pukekohe Maternity Resource Centre.
“She was president of the New Zealand Nurses Organisation Franklin Branch. She was involved with negotiations for pay parity for nurses and midwives and assisted the Ministry of Health to set up a structure for midwives providing lead maternity care.
“She was NZNO representative to the New Zealand Council of Women.”