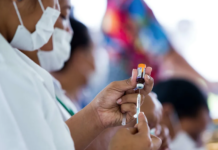
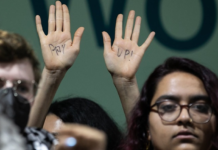A Pacific public health expert says a premature transition of covid-19 restrictions in New Zealand could be lethal for Māori and Pasifika communities.
The government is under increasing pressure to ease restrictions in Auckland with National saying it would set a six-week deadline for ending lockdowns and that a target of 85-90 percent vaccination rates were “do-able” within that timeframe.
Prime Minister Jacinda Ardern on Monday revealed the city would remain in alert level 3, step 1, and signalled the government would reveal a covid-19 protection plan on Friday.
- READ MORE: Covid-19 “tsunami coming”: Emergency nurse says lack of planning causing anxiety
- Other NZ covid lockdown reports
But Auckland University public health associate professor Collin Tukuitonga said easing restrictions before vaccination rates among the most at risk communities of Māori and Pasifika were high could be a death sentence.
“It is abundantly clear that Māori and Pasifika people will have more infections, more of them will go to hospital and more of them will die,” he said.
“Fortunately we haven’t had the deaths here that has been apparent in other countries. But clearly if we move prematurely the people at risk will pay the price.”
Hospitals ‘not ready for covid-19 tsunami’
Meanwhile, an Auckland emergency nurse and nursing union delegate told RNZ Morning Report today that overworked nurses feared hospitals were not ready for the “covid-19 tsunami” – and often thought about quitting.
Hospital admissions have climbed to 43, and Middlemore Hospital expects to see 20 cases a day through its emergency department next month.
The Ministry of Health yesterday reported 60 new community cases, a drop from Tuesday’s record 94 cases.
The nurse, who works in one of Auckland’s emergency departments (ED), said many of her colleagues finish shifts wondering if they would come back for the next one.
“The nurses are really, really feeling it – feeling really anxious. They feel like there’s a tsumani coming. They can see it coming … and what do they do? Do they run towards it or do they back off?”
Her own ED was often short by three or four nurses, or a couple of health care assistants, a shift, she said.
“On a daily basis we are getting texts to say, ‘can you pick up this shift?’. It is becoming a dire situation right now,” she said.
It was made worse because staff regularly needed to isolate because they were case contacts, she said.
The nurse, a delegate for the Nurses’ Organisation, said that if they could not staff the shifts, it made for a high pressure day for those left behind, she said.
This article is republished under a community partnership agreement with RNZ.