
An Auckland nurse says a lucrative incentive payment has not fixed the city’s dire hospital staffing shortage in Aotearoa New Zealand’s current covid-19 outbreak.
Nurses, midwives and others employed by the region’s district health boards (DHBs) have been entitled to an extra $500 on top of their normal pay for extra shifts overnight.
The scheme is being reviewed today and the clinical director in charge of co-ordinating the city’s health response, Dr Andrew Old, said it would continue if it was needed to address staffing shortages.
- LISTEN TO RNZ: ‘We’re in the eye of the storm now’ – Dr Andrew Old
- ‘We are tired, we are exhausted, we are short-staffed’ – Di McCulloch
- ‘The level of care you might expect [in hospital] is not as good’ – Sarah Dalton
- ‘It’s almost chaotic in terms of the response at this time’ – Tevita Funaki
- READ MORE: Ten deaths, 930 people in hospital, 19,566 new community cases
Dr Old said going into the pandemic Auckland’s hospitals had about 15 percent staff vacancies across the board which meant starting from a challenging position.
“So you then layer on top of that the challenge of Covid and it really has stretched the city.”
A nurses’ union delegate at Waitematā DHB, Di McCulloch, said while the $500 incentive scheme was popular, it had not been good for nursing overall because it led to exhausted workers and did not fix the staffing problems.
She said the nursing situation was dire.
Influx of unwell patients
“We continue to have an influx of unwell patients that normally enter the hospital and this has been compounded by omicron.”
She said once the subsidy ends the nursing shortages will continue and the DHBs will continue to redeploy non-clinical staff to fill the staffing gaps in wards.
Dr Old acknowledged how tired hospital staff in Auckland are.
“You know this has been going on for two years and the intensity has really stepped up in the last couple of weeks and I think certainly the city and the country are incredibly well served by the professionalism of the health workforce.”
Dr Old said the $500 payment was being reviewed today and there was the potential for it to be extended.
It aimed to ensure staff were available, particularly for hard to fill shifts such as overnights, he said.
“Look, we recognise people are tired, we’re asking them to go above and beyond and it’s just a recognition of the fact that actually everyone is really stretched.”
Hospitals just managing
Association of Salaried Medical Specialists executive director Sarah Dalton described the current situation as a crisis and said hospitals were only just managing.
“People are going above and beyond, they’re doing everything they can to keep it safe for patients, but that doesn’t mean it’s not a crisis, it doesn’t mean that the entrenched short staffing that we were trying to deal with before covid hasn’t made this almost impossible to deal with.”
It was not just Auckland and a lot of surgery and outpatient appointments were being cancelled around the country, she said.
McCulloch said the border closure had made the nursing shortages worse because in the past there had been a reliance on internationally qualified nurses (IQN).
“So it’s become an ongoing issue, this has been going on for years within nursing and the nursing voice are saying that we are tired, we are exhausted, we are short-staffed daily on the ground.”
But McCulloch said that had “not been heard by the powers that be”.
In terms of dealing with New Zealand’s ongoing nursing shortage, McCulloch said New Zealand needed to keep its new nursing graduates working here.
She said that could mean bonding newly qualified nurses to working in New Zealand for a minimum of two years.
Auckland hospitals put care on hold
Auckland hospitals have put all but the most urgent care on hold to allow them to focus on covid-19 patients.
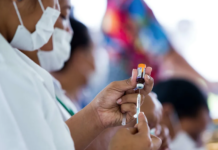
At the same time they are managing with 25 percent fewer staff as covid-19 cases continue to rise.
There were 19,566 cases and 930 people in hospital with the virus yesterday, more than two thirds of them in Auckland. Ten new covid-related deaths were also reported, taking the total to 151.
Dr Old said the region was grappling with peak hospitalisations and staff shortages due to the omicron outbreak.
“We’re in the eye of the storm now, so with cases thankfully coming down a bit but peak hospitalisations coinciding with near peak staff needing to be off to support their own family or off with covid themselves.”
But Dr Old said the number of staff vacancies due to covid-19 was starting to come down as coronavirus numbers start to drop and he was hopeful that things would improve this week.
He said there had been some limited cases of covid-19 positive staff working at Auckland hospital’s as the region dealt with the peak.
Serious challenges
“Those have been people where without them coming back we would have had serious challenges keeping those services going and so yes, coming back into environments where they’re only dealing with covid positive patients.”
Dalton said it was appalling to be in a position where in limited circumstances employers are encouraging staff unwell with covid-19 to go back to work.
“What they’re saying is they’re only doing that in covid settings and where otherwise there would be risk to life and limb effectively, so it’s a life preserving service.
“But to think that we’re in such a fragile state in terms of staffing that that has to be part of cover at the moment is really distressing.”
Dr Old stressed that urgent care was still available at the region’s hospitals.
“But anything that can be deferred essentially over the last couple of weeks really has been, so that’s pretty much all out-patient activity … and almost all planned surgery as well.”
Challenging to get support to South Auckland families
Auckland Pacific health and social service provider The Fono said it was run off its feet keeping up with the demands of a community struck by covid-19.
Chief executive Tevita Funaki said the service was looking after more than 900 active cases at one time.
“It’s not just the health challenges but also the whole welfare support and food and also other needs of the families.”
The service also had a number of staff getting sick or isolating due to covid-19.
The Fono had been using the network of churches in the Pacific community to distribute what was needed for families, Tevita said.
This article is republished under a community partnership agreement with RNZ.


![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-218x150.png)































![Andy Worthington: The startling severity of Gaza flotilla activists’ rape allegations "The [flotilla activists] were then illegally brought to Israel to face further abuse under the watch of Itamar Ben-Gvir, the terrorist thug serving as the Minister of National Security, who caused global outrage."](https://asiapacificreport.nz/wp-content/uploads/2026/05/Ben-Gvir-actists-AW-680wide-100x70.png)








